The implementation of PDPM in October is fast approaching and as we await the proposed rule, skilled nursing facility owners and operators are diligently preparing. One interesting bit of datum that I have been following closely surrounds the complexity of reimbursements associated with altered diets & swallowing problems in the SLP (Speech) Component.
Just to recap, under the Patient Driven Payment Model the newly developed SLP component has 12 distinct levels of reimbursement (see below). These levels are the result of answering five questions, and these questions are grouped into two separate (and differently weighted) groups. The second group has much more to do with eating chewing and swallowing.
The SLP Component Under PDPM
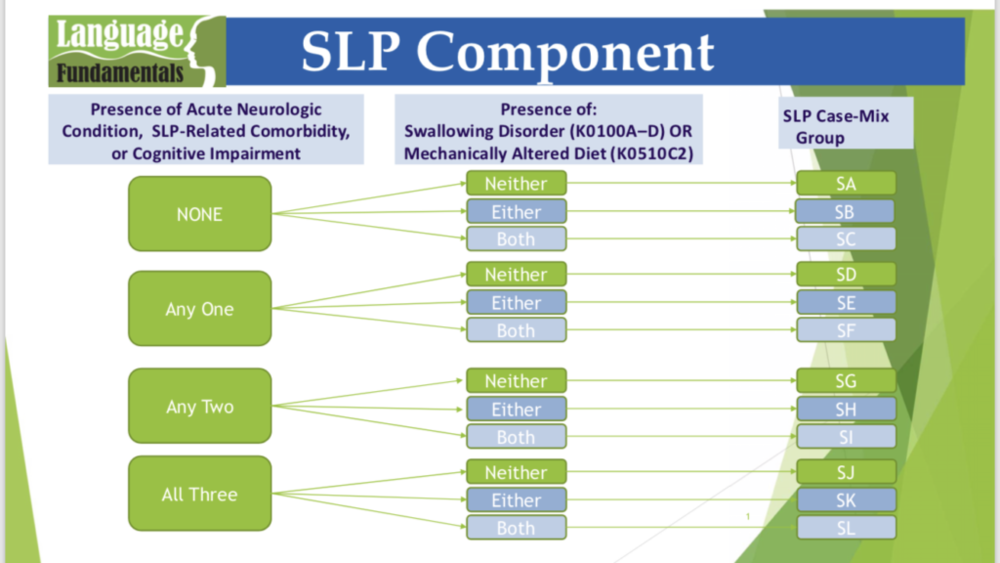
Group One:
1. Does patient’s primary diagnosis fall under acute neurologic or non-neurologic?
2. Is there an SLP related comorbidity?
3. Is there a moderate to severe cognitive impairment?
Group Two:
4. Is there a swallowing disorder?
5. Is the resident on an altered diet?
The answer to these questions will place the resident into one of 12 categories, SA-SL. If you guessed the “S” stands for super, you would be right. (Yes, it stands for speech but give that one to us)!
My main emphasis for this article is to demonstrate the importance of evaluating new residents for appropriate diets. Let’s illustrate with two different examples:
Resident A is medical management (non-neurologic) with no speech co-morbidities, is cognitively intact, has no swallowing issues, and is on a regular diet. Resident A will fall into the SA category. A SNF in Long Island, NY for example will receive $18.12 per day in the SLP category for each day of the Med A stay.
Resident B, on the other hand, is evaluated by a highly qualified SLP who can clearly document a swallowing dysfunction and consequently the need for an altered diet to ensure safe PO intake. Resident B will then fall into the SC category and the facility will receive $70.86 per day in the SLP category for each day of the Med A stay. A difference of $52.74 per day.
Over the course of that 30 day stay, the difference of $1,582.20 is significant. The difference between a highly skilled speech department and one that is less that proficient could be “make or break” under the PDPM.
In the next few months, speech therapy will focus on ensuring residents are getting the best care possible. We will also discuss accuracy of coding & the importance of strong supportive documentation. The importance of having coding & documentation that can survive future audits must not be forgotten in the PDPM transition.
Want to dive deeper on the SLP Component? Do you have ideas or questions? I’d love to talk. Please feel free to comment in the box below.



